 With the increasing prevalence of sexually transmissible diseases, syphilis has gained quite a lot of attention recently due to lasting health impacts. Syphilis is caused by the bacteria Treponema pallidum and is commonly transmitted through unprotected sexual contact with an infected person. In most cases, the condition is difficult to diagnose, as the bacteria can lie dormant years after initial infection. However, we must understand that if not treated on time, the condition can take a dangerous turn by promoting multiple organ failure in an advanced stage.
With the increasing prevalence of sexually transmissible diseases, syphilis has gained quite a lot of attention recently due to lasting health impacts. Syphilis is caused by the bacteria Treponema pallidum and is commonly transmitted through unprotected sexual contact with an infected person. In most cases, the condition is difficult to diagnose, as the bacteria can lie dormant years after initial infection. However, we must understand that if not treated on time, the condition can take a dangerous turn by promoting multiple organ failure in an advanced stage.
Stages of Syphilis Infection
Stating that, the causes for syphillis is sexually transmitting bacterial infection and is highly prevalent today. Most often the initial infection of syphilis often goes unnoticed. Depending upon the stages of infection, a person can exhibit multiple symptoms.
The primary stage of infection
Characteristic of this stage is either single and/or multiple painless, round-shape sores, often known as a chancre. These sores may last for almost six to eight weeks with and/or without treatment. Administration of timely treatment advisable at this stage to limit its progression to the secondary infection that is often more dangerous.
The secondary stage of infection
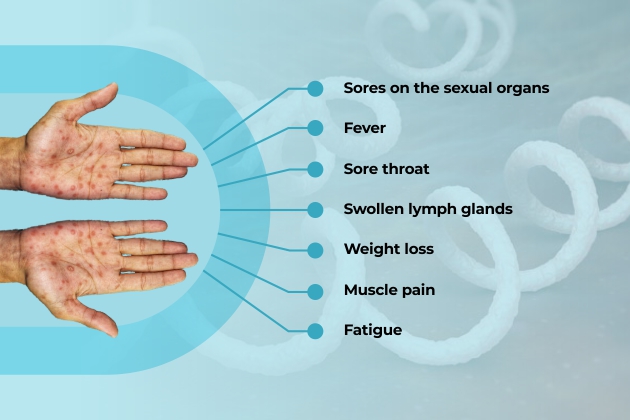
Apart from the presence of typical rash at more than one part of the body, this stage is often characterized by multiple other symptoms like
- Sores on the sexual organs
- Fever
- Sore throat
- Swollen lymph glands
- Weight loss
- Muscle pain
- Fatigue
If untreated at this stage, the infection can advance to the tertiary phase of infection
The tertiary stage of infection
This is the most advanced stage of infection. Generally, 30-40% of the people not getting treatment at right time can develop the same. People with this stage of infection suffer from dementia, mental fog, severe headache, cardiovascular issues, and paralysis.
Causes And Risk Factors of Syphilis
As already explained, syphilis causing bacteria enters the body through direct contact with an infected person. It is important to note that the infection does not spread after using cloths, napkins, and other items of an infected person. On a general note, an individual who is involved in sexual intercourse with an infected person without using protection is at a higher risk of infection. Especially, women with advanced stage of infection can have a direct impact on their pregnancies as well as newborn babies and hence, are at increased risk.
Diagnosis and Prognosis
The infection with syphilis often goes latent for years and can turn out fatal at times. Thus, it is advised that people with active sexual life and who do not use any prescribed protection during intercourse should opt for a VDRL test to confirm infection.
Early as well as secondary syphilis is easily curable with timely administration of antibiotics; preventing it from damaging other organs. However, the damage associated with organs in the tertiary phase of infection is often irreversible.
 Hepatitis B viral infection
Hepatitis B viral infection If the symptoms last for longer than six months, it shows that the acute infection has reached the stage of chronic infection. Symptoms of chronic infections are:
If the symptoms last for longer than six months, it shows that the acute infection has reached the stage of chronic infection. Symptoms of chronic infections are:
 If you’ve been recently diagnosed with low levels of vitamin D, you might be wondering – how to overcome vitamin D deficiency? Don’t panic. If it makes you feel any better, nearly 1 billion people worldwide are vitamin D deficient.
If you’ve been recently diagnosed with low levels of vitamin D, you might be wondering – how to overcome vitamin D deficiency? Don’t panic. If it makes you feel any better, nearly 1 billion people worldwide are vitamin D deficient.
 Chronic kidney disease (CKD) is a condition that involves a gradual loss of kidney function. It leads to a buildup of fluids, wastes, or electrolytes in our body because kidneys cannot filter these wastes from the blood to urine. Some of the chronic
Chronic kidney disease (CKD) is a condition that involves a gradual loss of kidney function. It leads to a buildup of fluids, wastes, or electrolytes in our body because kidneys cannot filter these wastes from the blood to urine. Some of the chronic 
 If you have ever gone through the diagnostic evaluation of any autoimmune condition; you might know what is the anti-CCP test and what does it confirm? Recently, the prevalence of autoimmune diseases has increased significantly; probably due to advancements in diagnostic tests and innovation of many biomarkers.
If you have ever gone through the diagnostic evaluation of any autoimmune condition; you might know what is the anti-CCP test and what does it confirm? Recently, the prevalence of autoimmune diseases has increased significantly; probably due to advancements in diagnostic tests and innovation of many biomarkers.
 There are several possible causes; some go away without treatment while some persist to worsen over time if left untreated. For a better long-term outlook, early diagnosis, as well as treatment of hyperthyroidism, are of utmost importance.
There are several possible causes; some go away without treatment while some persist to worsen over time if left untreated. For a better long-term outlook, early diagnosis, as well as treatment of hyperthyroidism, are of utmost importance.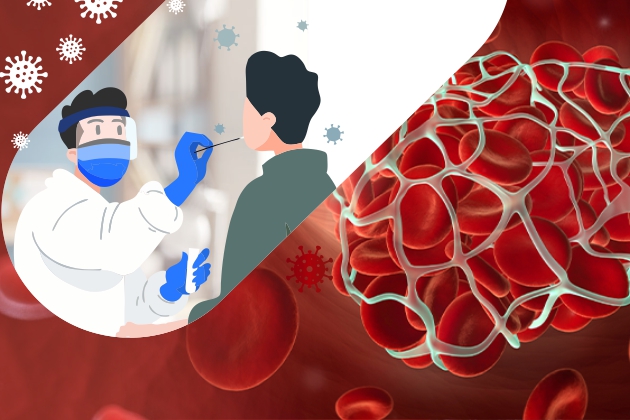
 While the globe is currently struggling with pandemic and survival through it; the diagnostic industry is also revamping continuously with many advancements and innovations in testing parameters, such as D-Dimer and COVID-19 tests. Although, nothing is truly rationalized about this disease of immunity and inflammation; scientists could associate elevated levels of certain biomarkers with the severity of infection and mortality trends. Read on to know everything about D-Dimer and how it can provide valuable insights on the inflammation associated with
While the globe is currently struggling with pandemic and survival through it; the diagnostic industry is also revamping continuously with many advancements and innovations in testing parameters, such as D-Dimer and COVID-19 tests. Although, nothing is truly rationalized about this disease of immunity and inflammation; scientists could associate elevated levels of certain biomarkers with the severity of infection and mortality trends. Read on to know everything about D-Dimer and how it can provide valuable insights on the inflammation associated with 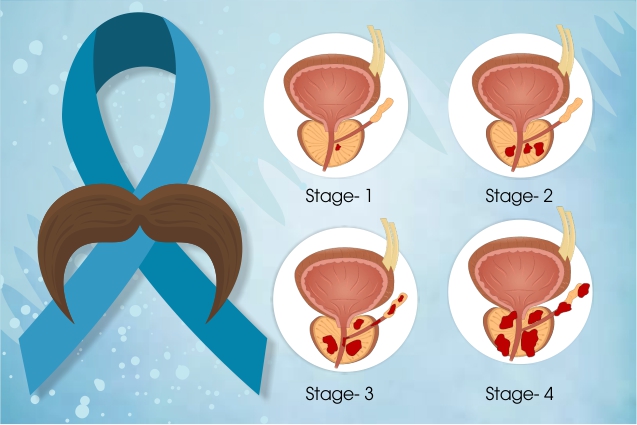
 Prostate cancer stages help doctors to determine how far cancer has spread and how best to treat it. Prostate cancer staging is a complex process that involves multiple tests, including
Prostate cancer stages help doctors to determine how far cancer has spread and how best to treat it. Prostate cancer staging is a complex process that involves multiple tests, including 


 Most people do not experience symptoms of kidney disease in the early stages of the disease. This is one of the reasons why in spite of the 10% population worldwide suffering from kidney disease, 90% of them are not aware that they have it. But, as the disease progresses, the kidney starts failing, and that’s when the kidney disease symptoms begin to show up.
Most people do not experience symptoms of kidney disease in the early stages of the disease. This is one of the reasons why in spite of the 10% population worldwide suffering from kidney disease, 90% of them are not aware that they have it. But, as the disease progresses, the kidney starts failing, and that’s when the kidney disease symptoms begin to show up.